At first I thought something was wrong with my kidney. So did my urologist. We were both convinced of it, because the symptoms sounded like it could be kidney stones, or perhaps even some kind of cancer. But the tests all came back negative. Dumbfounded, he suggested it might be muscular, said that sometimes pain in the hip or lower back can look a lot like kidney pain.
For those keeping track, my pain has manifested itself variously in my jaw, neck, groin, hip flexors, and now in the area around my right kidney. Before this post is over it will manifest in two more locations as well. This is one of the problems people have treating chronic pain that is due to structural issues in the body. The underlying causes might be the same, but they can manifest in different parts of the body at different times.
Even worse, specialists can be like the proverbial blind men appraising an elephant: each one sees a different part of the problem an advises accordingly. I was lucky that my urologist was thorough enough that he was able to rule out any urology issues, although that didn’t stop him from giving me some unnecessary pills.
Actually, my pain at this time was not just in the kidney region. I also was suffering from plantar fasciitis. There were two proximate causes for these problems, both due to having recently moved to Taipei. First of all, the move led to an interruption of my yoga practice. Secondly, the mattress in our new apartment was old and didn’t give me the support I needed. Once I realized that these were my old problems coming back in a new form I addressed both issues: finding a new Inyengar yoga studio in Taipei, and buying a better mattress from IKEA.
I also went to see a sports medicine doctor. This time I was lucky because the physical therapist I was assigned to was particularly good. In retrospect I can see that she was treating my problem in a way very close to what I finally realized was the correct approach. Unfortunately, the way physical therapy is done in Taiwan is largely about managing the symptoms, not fixing the root causes. So even though I had some good results, it wasn’t nearly enough. Still, it was a positive experience which would inform my thinking later on as I did more research.
It is worth mentioning one other thing I started to do at this time, and that is to see a tui-na specialist in Hualien. He has developed his own unique approach that mostly involved deep-tissue massage. Very painful, but effective. He is great, but no matter how good a massage is, it can only be a short term solution. Unless you get at the root of the problem you will continue to suffer from the same aches and pains and have to keep coming back for more.
Here I should pause to note again that I am not a doctor, physical therapist ,or personal trainer, I am just someone who has struggled to manage their own hip pain, but over the course of my research I have learned a lot, and I wanted to share those lessons with everyone. Please don’t take anything I write here as professional advice and consult a doctor before figuring out what to do in your own situation.
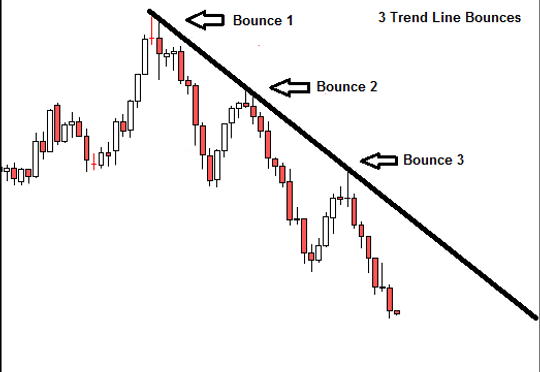
One problem with anyone who is running around seeking alternative treatments for a chronic pain or illness is that it is very hard to tell if something is working or not. Recovery and decline both have peaks and valleys, like the stock market, and one is much more attuned to those peaks and valleys than the overall trend line. We might think something is working (yoga, massage, acupuncture, etc.) because there is a slight improvement after each intervention, but the overall trend line might still be downwards.
Who knows, maybe my current success is just another illusion created by the peaks and valleys of pain and recovery, hiding the true downward trend? Maybe, but I don’t think so. This is why I started this series with objective goalposts and waited till I had achieved them before starting to write. For the years between my visit to the urologist and when I started my current approach, however, the trend was definitely downwards.
Between 2015 and 2019 I was doing everything I could think of, but my problems just kept getting worse. I was barely sleeping at night. That these years were also a period of intense stress due to my running an international film festival and trying to get promoted to full professor didn’t help. Thinking back, it is remarkable that I managed at all, but like I said, peaks and valleys: I wasn’t doing badly the entire time. Yoga, despite its limitations, kept me going.
But in 2018 the pain manifest in yet another location: my shins. Strangely, it only hurt at night. I went to see orthopedic surgeons at hospitals in Hualien and Taipei. In the months to follow I would do an MRI, multiple X-rays, and even a CT-scan. Doctors suggested and evaluated numerous possibilities: it might claudication from lack of blood flow, compartment syndrome in which the muscle doesn’t have room to grow, a fractured tibia (perhaps due to cancer), and all kinds of other possibilities. But pretty much everything was ruled out. It was only after this long period of testing was over that someone suggested the real cause might be in my hips.
This started another round of visits and testing, but this time the results were somewhat more conclusive. Based on x-rays, I was given two related diagnosis, both of which often occur together. One was “osteoarthritis,” in which the cartilage in the hip joint is worn away. The other was “femoroacetabular impingement” (FAI) in which bone spurs grow outside the hip joint, limiting one’s range of motion.
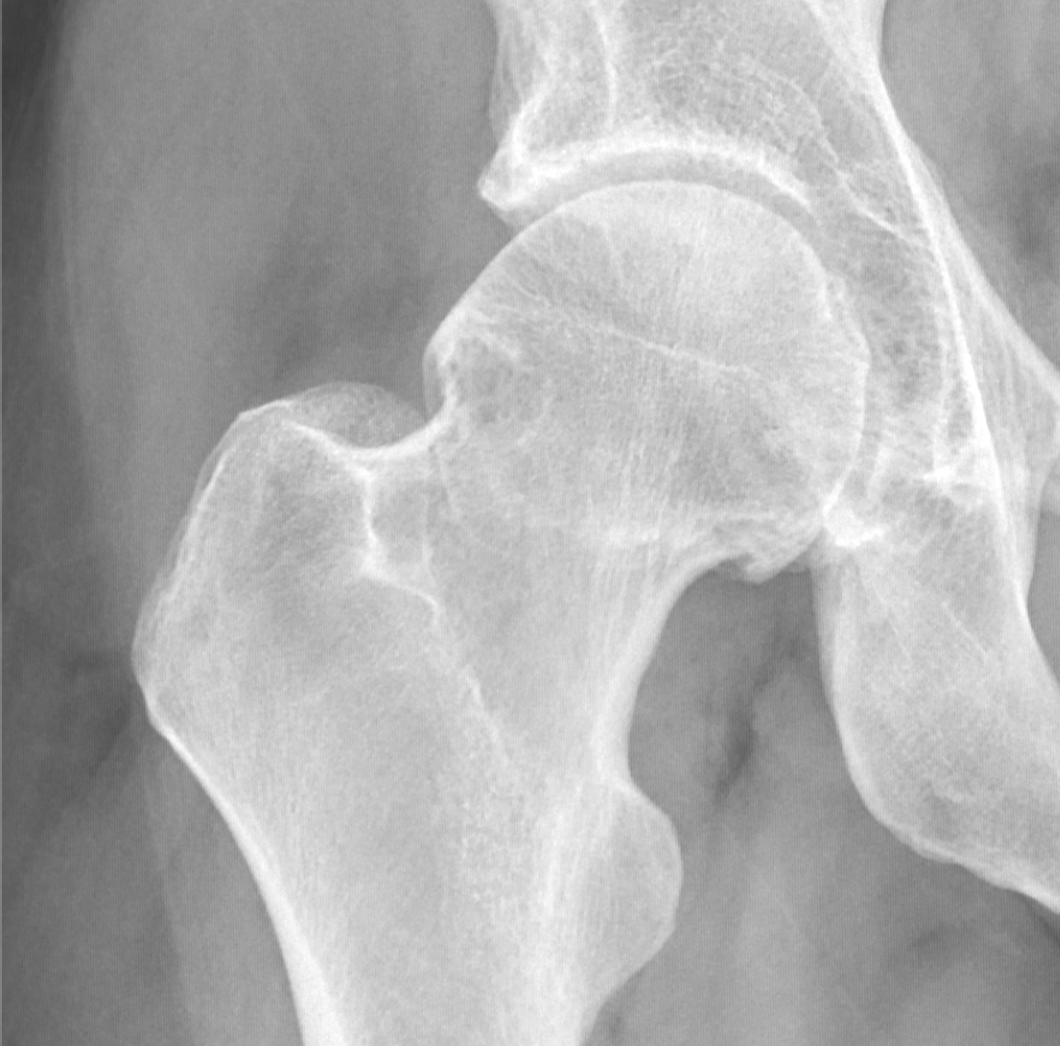
Some doctors recommended immediate surgery, others suggested I do more physical therapy. Some people even pointed me to new experimental treatments where they inject fluid with your own stem cells into the hip. Doing some research on my own I discovered that the success rates of these various surgical interventions weren’t very good, so I decided to stick with physical therapy for the present time. Again I had some short term relief, but was frustrated at not having a long-term plan to truly improve my situation. Here is where the diagnosis of FAI led to something of a breakthrough.
If you start searching for FAI on YouTube you will soon find this video from Matt Hsu at Upright health:
I am not exaggerating when I say that this video changed my life. I never signed up for any of the online courses Upright Health promotes (although I may do so just to repay them for helping me so much with their free videos), but this video really helped change my thinking about how to approach my problems.
One point Matt makes is that many people with no symptoms whatsoever have bone structures that look the same as people who are recommended to have surgery. In other words, having imagery of reduced cartilage and bone spurs is not necessarily a sign that you necessarily need to have surgery. Everyone will be different, but (so far, at least) this turned out to be true for me. In my next post I will turn to the combination of practices I started to explore after seeing this video, and why I think they work.
